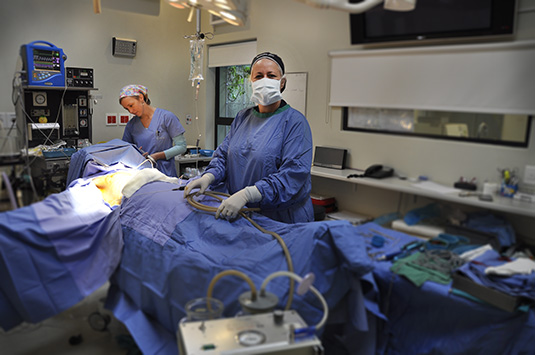
Your Surgery – What to expect
This is your big day. Expect to be anxious, nervous or afraid. We will give you a pre-med sedative to help with this. For my staff and I this is what we do every day. For us this is routine and we will help you through it. We will try to set you at ease from the start and, in fact, the day, especially the early part when the surgery occurs, will pass in a bit of blur. The drugs we give you will make you calm, relaxed and sleepy.
If you are the first case of the day we will want you at the clinic at 7.30 am. Otherwise we will give you a time to arrive. Usually we will want you starved from 2 am which for most patients means nothing to eat or drink after you wake. You can brush your teeth.
You will usually be admitted to the ward by Elmare, my general nurse. If we are using an anaesthetist (most body surgery) then the anaesthetist will introduce herself to you and discuss the anaesthesia or sedation that you will have. I will mark you up in the ward (draw on you with permanent surgical marker) and check that you are comfortable and ready.
Most of my surgery is performed as day case surgery (in and out the same day) under twilight sedation in my own ambulatory plastic surgery facility. Once marked, I will take you through to theatre and hand you over to the anaesthetist. They will ensure that during the procedure you are asleep, pain-free and unaware of surgery. I use an anaesthetist for almost all body procedures including liposuction, breast and tummy surgery. For most facial work, however, I administer the sedation myself and use local anaesthetic. This is a very comfortable and gentle way to have surgery.
Once anaesthetised, I perform the surgery. I am a careful and conservative surgeon preferring conventional, tried and tested procedures. I would rather spend an extra few minutes making sure everything is okay than return later that night to deal with a problem. Wounds are usually closed with dissolving sutures. Drains are infrequently used. Light dressings and support garments are usually applied at the end of the procedure. Pain killers are given for your recovery.
Following the surgery you will recover in the ward. We will continue to give you pain killers and anti nausea medication as required. The nurses will monitor you as you recover and I will be around and check on you from time to time. You will not be discharged until you are up and about, walking, talking and have passed urine. Usually we will want to discharge you into the company of a responsible adult. Painkillers and detailed instructions will be given on discharge.
I will see you for follow up a day or two after surgery and then regularly after that. Follow up consultations are not charged for and I have an open door policy – if ever you experience any issue with the operative site I will see you without charge.